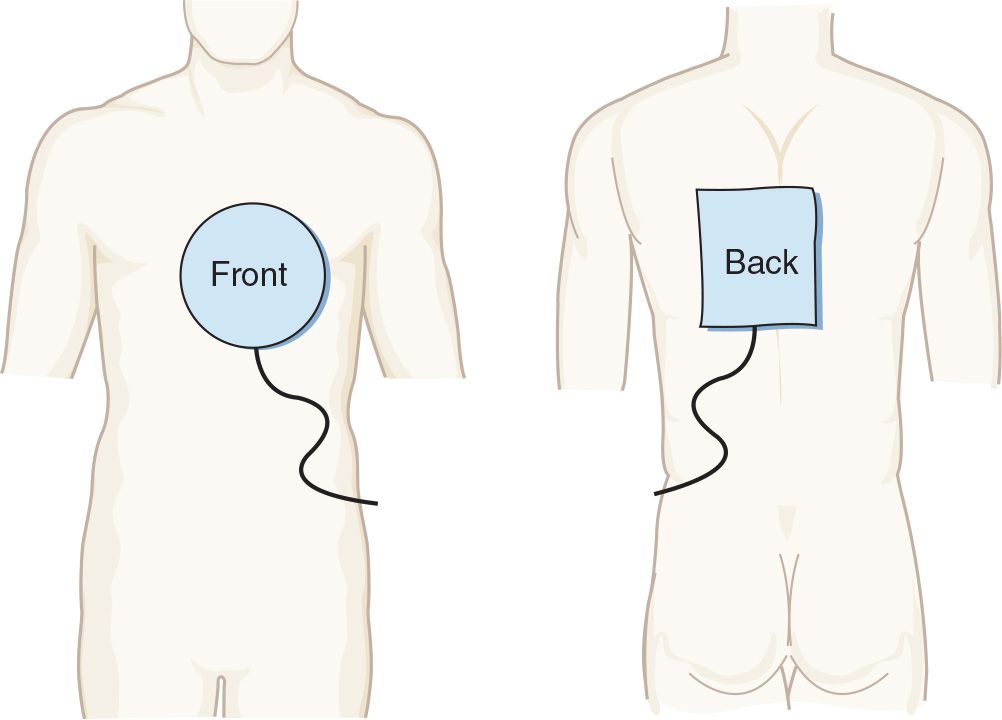
Methods to identify the manufacturer include review of the pacing system identification card that all patients should carry, review of medical records that identify the pacemaker manufacturer, or radiographic identification. However, interrogation requires knowing the pulse generator manufacturer, because pulse generators only communicate with programmers made by the same manufacturer. The first step in troubleshooting is pacemaker interrogation. 
It is also very useful (but sometimes difficult) to obtain the chest radiograph taken immediately after implantation for comparison with current radiographs (see Chapter 11: Radiography of Implantable Devices). Table 10.2 Toll-free, 24-h telephone numbers of manufacturers. (If calling for implant information ask for “patient registration” and if calling for troubleshooting assistance ask for “brady technical support”.) The manufacturers can also provide technical information about device and lead performance and assist with electrocardiographic interpretation and troubleshooting. All manufacturers have toll-free numbers that may be used to obtain implant information (generally kept by the manufacturer of the pulse generator), such as device model and lead models ( Table 10.2). Many devices store information on lead models, acute threshold data, clinical information (e.g., medication regimen), name of institution where the device was implanted, and name of the implanting physician in their memory, for retrieval upon interrogation. It is important to obtain information from the operative report if possible, including device model, lead models, acute intraoperative pacing and sensing thresholds, and impedance values, and any difficulties encountered during implantation. During routine follow-up, the patient should be asked about symptoms potentially related to pacemaker complications, such as recurrence of preimplant symptoms, syncope, near-syncope, palpitations, and any perception of a slow, fast, or irregular pulse. For example, intermittent failure to capture in the nonpacemaker-dependent patient or undersensing may not be associated with any symptoms and may be discovered only at the time of routine evaluation. Some types of pacing system malfunctions may occur totally without symptoms. Symptoms of pacing system malfunction may be subtle and include fatigue, weakness, confusion, neck pulsations, or activity intolerance. Clinical assessment should include the following information: the original indication for pacing, whether or not the patient is pacemaker-dependent, activity immediately preceding the clinical event, symptoms experienced by the patient during the event, observations made by witnesses, and duration of the event. Knowing the patient and taking a careful history are very important in evaluating any pacing system, especially if malfunction is suspected. The most common problems encountered in pacemaker management include: In order to adopt a systematic approach to troubleshooting, an understanding of the common problems encountered in a device clinic and their causes is necessary. 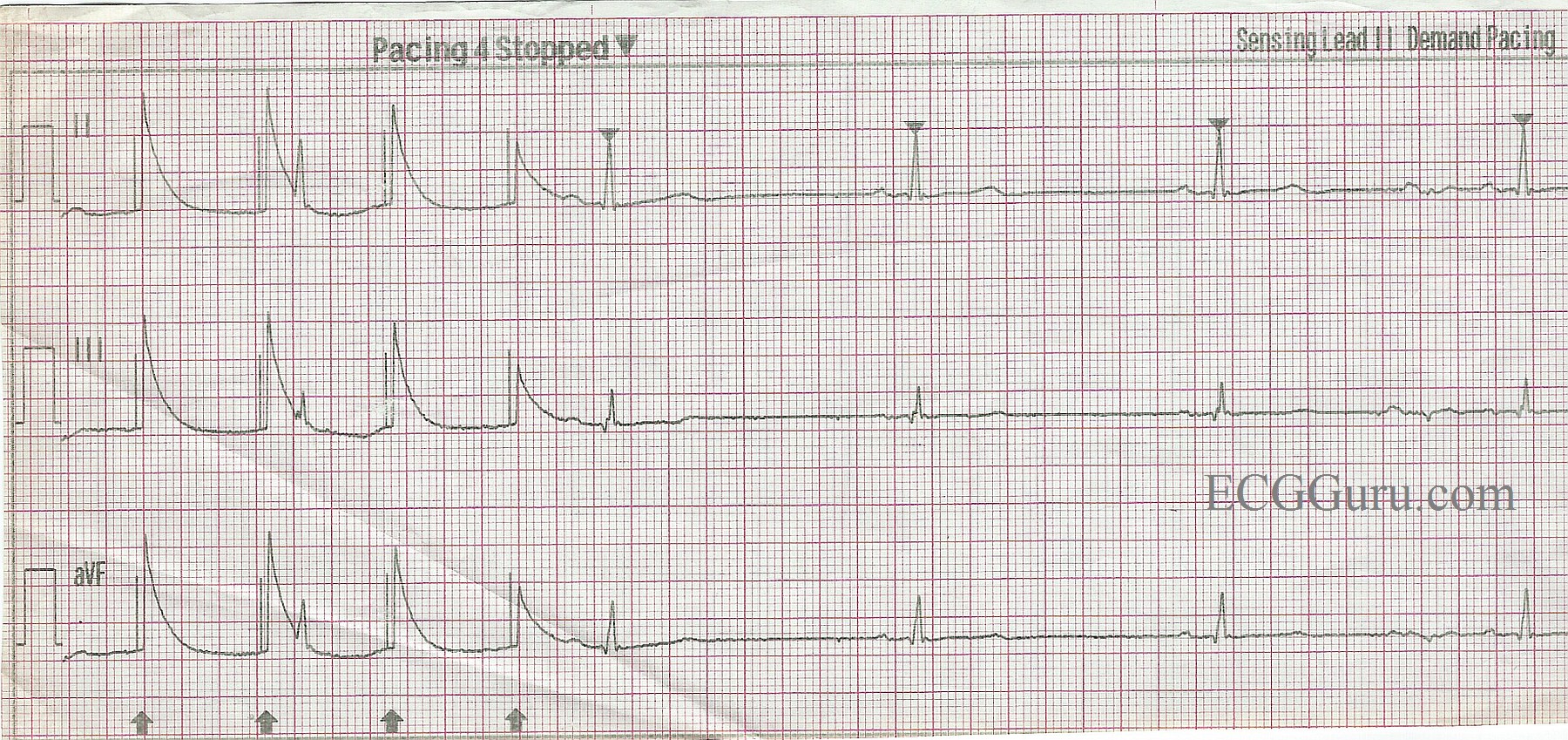
Review technical manual for other “clues” to perceived malfunction Proper contact between lead pins and setscrews If noninvasive evaluation is unrewarding, operative assessment may be necessary. Before invasive troubleshooting, one should take advantage of every possible source of assistance, including careful review of the technical manual and contacting the manufacturer for help. Noninvasive diagnosis and correction of any malfunction are always preferable to operative management. Noninvasive evaluation should be exhausted first and involve careful evaluation of any symptoms the pacing indication available electrocardiographic tracings the function and radiographic appearance of the lead system and stored information obtained by telemetry from the pulse generator. Successful troubleshooting requires a systematic approach ( Table 10.1). In some instances, early component failure is intermittent, and even meticulous evaluation of the system may not initially reveal a problem. Some instances of device “malfunction” are not malfunctions at all, but rather are the result of an inappropriately programmed device functioning as programmed or unrecognized appropriate function, i.e., pseudo-malfunction. Whether a patient has a clinical episode that suggests system malfunction or is having routine follow-up, device evaluation should be performed in an orderly fashion so that potential malfunction is not overlooked. Knowledge of the device capabilities and the clinical situation of the patient is key to successful troubleshooting. Pacemaker diagnostics and automaticity have become increasingly more sophisticated.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
